-
Ortho Micronor Tablets (Ortho Women's Health & Urology)
Prescribing Information
Patients should be counseled that this product does not protect against HIV infection (AIDS) and other sexually transmitted diseases.
DESCRIPTION
ORTHO MICRONOR® 28 Day Regimen
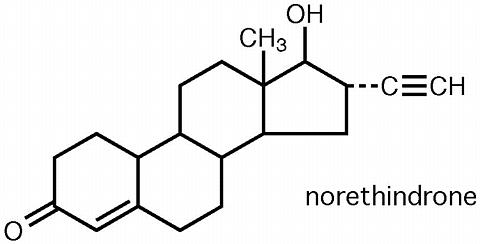
Each tablet contains 0.35 mg norethindrone. Inactive ingredients include D&C Green No. 5, D&C Yellow No. 10, lactose, magnesium stearate, povidone and starch.
CLINICAL PHARMACOLOGY
-
MODE OF ACTION
ORTHO MICRONOR progestin-only oral contraceptives prevent conception by suppressing ovulation in approximately half of users, thickening the cervical mucus to inhibit sperm penetration, lowering the midcycle LH and FSH peaks, slowing the movement of the ovum through the fallopian tubes, and altering the endometrium. -
PHARMACOKINETICS
Serum progestin levels peak about two hours after oral administration, followed by rapid distribution and elimination. By 24 hours after drug ingestion, serum levels are near baseline, making efficacy dependent upon rigid adherence to the dosing schedule. There are large variations in serum levels among individual users. Progestin-only administration results in lower steady-state serum progestin levels and a shorter elimination half-life than concomitant administration with estrogens.
INDICATIONS AND USAGE
-
Indications
Progestin-only oral contraceptives are indicated for the prevention of pregnancy. -
Efficacy
If used perfectly, the first-year failure rate for progestin-only oral contraceptives is 0.5%. However, the typical failure rate is estimated to be closer to 5%, due to late or omitted pills. Table 1 lists the pregnancy rates for users of all major methods of contraception.
TABLE 1: PERCENTAGE OF WOMEN EXPERIENCING
AN UNINTENDED PREGNANCY DURING THE FIRST YEAR OF TYPICAL USE
AND THE FIRST YEAR OF PERFECT USE OF CONTRACEPTION
AND THE PERCENTAGE CONTINUING USE AT THE END OF THE FIRST YEAR.
UNITED STATES.% of Women Experiencing an
Unintended Pregnancy
within the First Year of Use% of Women
Continuing Use
at One Year 3Method
(1)Typical Use 1
(2)Perfect Use 2
(3)(4) Chance 485 85 Spermicides 526 6 40 Periodic abstinence25 63 Calendar9 Ovulation Method3 Sympto-Thermal 62 Post-Ovulation1 Withdrawal19 4 Cap 7Parous Women40 26 42 Nulliparous Women20 9 56 SpongeParous Women40 20 42 Nulliparous Women20 9 56 Diaphragm 720 6 56 Condom 8Female (Reality)21 5 56 Male14 3 61 Pill5 71 Progestin Only0.5 Combined0.1 IUDProgesterone T2.0 1.5 81 Copper T380A0.8 0.6 78 LNg 200.1 0.1 81 Depo-Provera0.3 0.3 70 Norplant and Norplant-20.05 0.05 88 Female Sterilization0.5 0.5 100 Male Sterilization0.15 0.10 100 Adapted from Trussel J. Contraceptive efficacy. In Hatcher RA, Trussel J, Stewart F, Cates W, Stewart GK, Kowal D, Guest F, Contraceptive Technology: Seventeenth Revised Edition. New York NY: Irvington Publishers, 1998, in press.
1. Among typical couples who initiate use of a method (not necessarily for the first time), the percentage who experience an accidental pregnancy during the first year if they do not stop use for any other reason.2. Among couples who initiate use of a method (not necessarily for the first time) and who use it perfectly (both consistently and correctly), the percentage who experience an accidental pregnancy during the first year if they do not stop use for any other reason.3. Among couples attempting to avoid pregnancy, the percentage who continue to use a method for one year.4. The percents becoming pregnant in columns (2) and (3) are based on data from populations where contraception is not used and from women who cease using contraception in order to become pregnant. Among such populations, about 89% become pregnant within one year. This estimate was lowered slightly (to 85%) to represent the percent who would become pregnant within one year among women now relying on reversible methods of contraception if they abandoned contraception altogether.5. Foams, creams, gels, vaginal suppositories, and vaginal film.6. Cervical mucus (ovulation) method supplemented by calendar in the pre-ovulatory and basal body temperature in the post-ovulatory phases.7. With spermicidal cream or jelly.8. Without spermicides.CONTRAINDICATIONS
Progestin-only oral contraceptives (POPs) should not be used by women who currently have the following conditions:
- Known or suspected pregnancy
- Known or suspected carcinoma of the breast
- Undiagnosed abnormal genital bleeding
- Hypersensitivity to any component of this product
- Benign or malignant liver tumors
- Acute liver disease
WARNINGS
Cigarette smoking increases the risk of serious cardiovascular disease. Women who use oral contraceptives should be strongly advised not to smoke.
ORTHO MICRONOR does not contain estrogen and, therefore, this insert does not discuss the serious health risks that have been associated with the estrogen component of combined oral contraceptives (COCs). The health care provider is referred to the prescribing information of combined oral contraceptives for a discussion of those risks. The relationship between progestin-only oral contraceptives and these risks is not fully defined. The physician should remain alert to the earliest manifestation of symptoms of any serious disease and discontinue oral contraceptive therapy when appropriate.
-
Ectopic Pregnancy
The incidence of ectopic pregnancies for progestin-only oral contraceptive users is 5 per 1000 woman-years. Up to 10% of pregnancies reported in clinical studies of progestin-only oral contraceptive users are extrauterine. Although symptoms of ectopic pregnancy should be watched for, a history of ectopic pregnancy need not be considered a contraindication to use of this contraceptive method. Health providers should be alert to the possibility of an ectopic pregnancy in women who become pregnant or complain of lower abdominal pain while on progestin-only oral contraceptives. -
Delayed Follicular Atresia/Ovarian Cysts
If follicular development occurs, atresia of the follicle is sometimes delayed and the follicle may continue to grow beyond the size it would attain in a normal cycle. Generally these enlarged follicles disappear spontaneously. Often they are asymptomatic; in some cases they are associated with mild abdominal pain. Rarely they may twist or rupture, requiring surgical intervention. -
Irregular Genital Bleeding
Irregular menstrual patterns are common among women using progestin-only oral contraceptives. If genital bleeding is suggestive of infection, malignancy or other abnormal conditions, such nonpharmacologic causes should be ruled out. If prolonged amenorrhea occurs, the possibility of pregnancy should be evaluated. -
Carcinoma of the Breast and Reproductive Organs
Some epidemiological studies of oral contraceptive users have reported an increased relative risk of developing breast cancer, particularly at a younger age and apparently related to duration of use. These studies have predominantly involved combined oral contraceptives and there is insufficient data to determine whether the use of POPs similarly increases the risk.
A meta-analysis of 54 studies found a small increase in the frequency of having breast cancer diagnosed for women who were currently using combined oral contraceptives or had used them within the past ten years. This increase in the frequency of breast cancer diagnosis, within ten years of stopping use, was generally accounted for by cancers localized to the breast. There was no increase in the frequency of having breast cancer diagnosed ten or more years after cessation of use.
Women with breast cancer should not use oral contraceptives because the role of female hormones in breast cancer has not been fully determined.
Some studies suggest that oral contraceptive use has been associated with an increase in the risk of cervical intraepithelial neoplasia in some populations of women. However, there continues to be controversy about the extent to which such findings may be due to differences in sexual behavior and other factors. There is insufficient data to determine whether the use of POPs increases the risk of developing cervical intraepithelial neoplasia. -
Hepatic Neoplasia
Benign hepatic adenomas are associated with combined oral contraceptive use, although the incidence of benign tumors is rare in the United States. Rupture of benign, hepatic adenomas may cause death through intraabdominal hemorrhage.
Studies have shown an increased risk of developing hepatocellular carcinoma in combined oral contraceptive users. However, these cancers are rare in the U.S. There is insufficient data to determine whether POPs increase the risk of developing hepatic neoplasia.
PRECAUTIONS
1. General
Patients should be counseled that this product does not protect against HIV infection (AIDS) and other sexually transmitted diseases.
2. Physical Examination and Follow up
It is considered good medical practice for sexually active women using oral contraceptives to have annual history and physical examinations. The physical examination may be deferred until after initiation of oral contraceptives if requested by the woman and judged appropriate by the clinician.
3. Carbohydrate and Lipid Metabolism
Some users may experience slight deterioration in glucose tolerance, with increases in plasma insulin but women with diabetes mellitus who use progestin-only oral contraceptives do not generally experience changes in their insulin requirements. Nonetheless, prediabetic and diabetic women in particular should be carefully monitored while taking POPs.
Lipid metabolism is occasionally affected in that HDL, HDL2, and apolipoprotein A-I and A-II may be decreased; hepatic lipase may be increased. There is usually no effect on total cholesterol, HDL 3 , LDL, or VLDL.
4. Drug Interactions
The effectiveness of progestin-only pills is reduced by hepatic enzyme-inducing drugs such as the anticonvulsants phenytoin, carbamazepine, and barbiturates, and the antituberculosis drug rifampin. No significant interaction has been found with broad-spectrum antibiotics.
5. Interactions with Laboratory Tests
The following endocrine tests may be affected by progestin-only oral contraceptive use:
- Sex hormone-binding globulin (SHBG) concentrations may be decreased.
- Thyroxine concentrations may be decreased, due to a decrease in thyroid binding globulin (TBG).
6. Carcinogenesis
See WARNINGS section.
7. Pregnancy
Many studies have found no effects on fetal development associated with long-term use of contraceptive doses of oral progestins. The few studies of infant growth and development that have been conducted have not demonstrated significant adverse effects. It is nonetheless prudent to rule out suspected pregnancy before initiating any hormonal contraceptive use.
8. Nursing Mothers
No adverse effects have been found on breastfeeding performance or on the health, growth or development of the infant. Small amounts of progestin pass into the breast milk, resulting in steroid levels in infant plasma of 1-6% of the levels of maternal plasma.
9. Pediatric Use
Safety and efficacy of ORTHO MICRONOR Tablets have been established in women of reproductive age. Safety and efficacy are expected to be the same for postpubertal adolescents under the age of 16 and for users 16 years and older. Use of this product before menarche is not indicated.
10. Fertility Following Discontinuation
The limited available data indicate a rapid return of normal ovulation and fertility following discontinuation of progestin-only oral contraceptives.
11. Headache
The onset or exacerbation of migraine or development of severe headache with focal neurological symptoms which is recurrent or persistent requires discontinuation of progestin-only contraceptives and evaluation of the cause.
INFORMATION FOR THE PATIENT
- See Detailed Patient Labeling for detailed information.
- Counseling issues
The following points should be discussed with prospective users before prescribing progestin-only oral contraceptives:
- The necessity of taking pills at the same time every day, including throughout all bleeding episodes.
- The need to use a backup method such as condoms and spermicides for the next 48 hours whenever a progestin-only oral contraceptive is taken 3 or more hours late.
- The potential side effects of progestin-only oral contraceptives, particularly menstrual irregularities.
- The need to inform the clinician of prolonged episodes of bleeding, amenorrhea or severe abdominal pain.
- The importance of using a barrier method in addition to progestin-only oral contraceptives if a woman is at risk of contracting or transmitting STDs/HIV.
ADVERSE REACTIONS
Adverse reactions reported with the use of POPs include:
- Menstrual irregularity is the most frequently reported side effect.
- Frequent and irregular bleeding are common, while long duration of bleeding episodes and amenorrhea are less likely.
- Headache, breast tenderness, nausea, and dizziness are increased among progestin-only oral contraceptive users in some studies.
- Androgenic side effects such as acne, hirsutism, and weight gain occur rarely.
OVERDOSAGE
There have been no reports of serious ill effects from overdosage, including ingestion by children.
DOSAGE AND ADMINISTRATION
To achieve maximum contraceptive effectiveness, ORTHO MICRONOR must be taken exactly as directed. One tablet is taken every day, at the same time. Administration is continuous, with no interruption between pill packs. See Detailed Patient Labeling for detailed instruction.
HOW SUPPLIED
ORTHO MICRONOR Tablets are available in a DIALPAK® Tablet Dispenser
(NDC 0062-1411-16) containing 28 green tablets (0.35 mg norethindrone).
STORAGE: Store at 25°C (77°F); excursions permitted to 15°-30°C (59-86°F).
REFERENCE
McCann M, and Potter L. Progestin-Only Oral Contraceptives: A Comprehensive Review. Contraception, 50:60 (Suppl. 1), December 1994.
DETAILED PATIENT LABELING
ORTHO MICRONOR® (norethindrone) Tablets
This product (like all oral contraceptives) is used to prevent pregnancy. It does not protect against HIV infection (AIDS) or other sexually transmitted diseases.
DESCRIPTION
ORTHO MICRONOR® 28 Day Regimen
Each tablet contains 0.35 mg norethindrone. Inactive ingredients include D&C Green No. 5, D&C Yellow No. 10, lactose, magnesium stearate, povidone and starch.
INTRODUCTION
This leaflet is about birth control pills that contain one hormone, a progestin. Please read this leaflet before you begin to take your pills. It is meant to be used along with talking with your doctor or clinic.
Progestin-only pills are often called "POPs" or "the minipill." POPs have less progestin than the combined birth control pill (or "the pill") which contains both an estrogen and a progestin.
HOW EFFECTIVE ARE POPs?
About 1 in 200 POP users will get pregnant in the first year if they all take POPs perfectly (that is, on time, every day). About 1 in 20 "typical" POP users (including women who are late taking pills or miss pills) gets pregnant in the first year of use. Table 2 will help you compare the efficacy of different methods.
TABLE 2: PERCENTAGE OF WOMEN EXPERIENCING
AN UNINTENDED PREGNANCY DURING THE FIRST YEAR OF TYPICAL USE
AND THE FIRST YEAR OF PERFECT USE OF CONTRACEPTION
AND THE PERCENTAGE CONTINUING USE AT THE END OF THE FIRST YEAR.
UNITED STATES.% of Women Experiencing an
Unintended Pregnancy
within the First Year of Use% of Women
Continuing Use
at One Year 3Method
(1)Typical Use 1
(2)Perfect Use 2
(3)(4) Chance 485 85 Spermicides 526 6 40 Periodic abstinence25 63 Calendar9 Ovulation Method3 Sympto-Thermal 62 Post-Ovulation1 Withdrawal19 4 Cap 7Parous Women40 26 42 Nulliparous Women20 9 56 SpongeParous Women40 20 42 Nulliparous Women20 9 56 Diaphragm20 6 56 Condom 8Female (Reality)21 5 56 Male14 3 61 Pill5 71 Progestin Only0.5 Combined0.1 IUDProgesterone T2.0 1.5 81 Copper T380A0.8 0.6 78 LNg 200.1 0.1 81 Depo-Provera0.3 0.3 70 Norplant and Norplant-20.05 0.05 88 Female Sterilization0.5 0.5 100 Male Sterilization0.15 0.10 100 Adapted from Trussel J. Contraceptive efficacy. In Hatcher RA, Trussel J, Stewart F, Cates W, Stewart GK, Kowal D, Guest F, Contraceptive Technology: Seventeenth Revised Edition. New York NY: Irvington Publishers, 1998, in press.
1. Among typical couples who initiate use of a method (not necessarily for the first time), the percentage who experience an accidental pregnancy during the first year if they do not stop use for any other reason.2. Among couples who initiate use of a method (not necessarily for the first time) and who use it perfectly (both consistently and correctly), the percentage who experience an accidental pregnancy during the first year if they do not stop use for any other reason.3. Among couples attempting to avoid pregnancy, the percentage who continue to use a method for one year.4. The percents becoming pregnant in columns (2) and (3) are based on data from populations where contraception is not used and from women who cease using contraception in order to become pregnant. Among such populations, about 89% become pregnant within one year. This estimate was lowered slightly (to 85%) to represent the percent who would become pregnant within one year among women now relying on reversible methods of contraception if they abandoned contraception altogether.5. Foams, creams, gels, vaginal suppositories, and vaginal film.6. Cervical mucus (ovulation) method supplemented by calendar in the pre-ovulatory and basal body temperature in the post-ovulatory phases.7. With spermicidal cream or jelly.8. Without spermicides.HOW DO POPs WORK?
POPs can prevent pregnancy in different ways including:
- They make the cervical mucus at the entrance to the womb (the uterus) too thick for the sperm to get through to the egg.
- They prevent ovulation (release of the egg from the ovary) in about half of the cycles.
- They also affect other hormones, the fallopian tubes and the lining of the uterus.
YOU SHOULD NOT TAKE POPs
- If there is any chance you may be pregnant.
- If you have breast cancer.
- If you have bleeding between your periods that has not been diagnosed.
- If you are taking certain drugs for epilepsy (seizures) or for TB. (See "Using POPs with Other Medicines" below.)
- If you are hypersensitive, or allergic, to any component of this product.
- If you have liver tumors, either benign or cancerous.
- If you have acute liver disease.
RISKS OF TAKING POPs
Cigarette smoking greatly increases the possibility of suffering heart attacks and strokes. Women who use oral contraceptives are strongly advised not to smoke.
WARNING: If you have sudden or severe pain in your lower abdomen or stomach area, you may have an ectopic pregnancy or an ovarian cyst. If this happens, you should contact your doctor or clinic immediately.
Ectopic Pregnancy
An ectopic pregnancy is a pregnancy outside the womb. Because POPs protect against pregnancy, the chance of having a pregnancy outside the womb is very low. If you do get pregnant while taking POPs, you have a slightly higher chance that the pregnancy will be ectopic than do users of some other birth control methods.
Ovarian Cysts
These cysts are small sacs of fluid in the ovary. They are more common among POP users than among users of most other birth control methods. They usually disappear without treatment and rarely cause problems.
Cancer of the Reproductive Organs and Breasts
Some studies in women who use combined oral contraceptives that contain both estrogen and a progestin have reported an increase in the risk of developing breast cancer, particularly at a younger age and apparently related to duration of use. There is insufficient data to determine whether the use of POPs similarly increases this risk.
A meta-analysis of 54 studies found a small increase in the frequency of having breast cancer diagnosed for women who were currently using combined oral contraceptives or had used them within the past ten years. This increase in the frequency of breast cancer diagnosis, within ten years of stopping use, was generally accounted for by cancers localized to the breast. There was no increase in the frequency of having breast cancer diagnosed ten or more years after cessation of use.
Some studies have found an increase in the incidence of cancer of the cervix in women who use oral contraceptives. However, this finding may be related to factors other than the use of oral contraceptives and there is insufficient data to determine whether the use of POPs increases the risk of developing cancer of the cervix.
Liver Tumors
In rare cases, combined oral contraceptives can cause benign but dangerous liver tumors. These benign liver tumors can rupture and cause fatal internal bleeding. In addition, some studies report an increased risk of developing liver cancer among women who use combined oral contraceptives. However, liver cancers are rare. There is insufficient data to determine whether POPs increase the risk of liver tumors.
Diabetic Women
Diabetic women taking POPs do not generally require changes in the amount of insulin they are taking. However, your physician may monitor you more closely under these conditions.
SEXUALLY TRANSMITTED DISEASES (STDs)
WARNING: POPs do not protect against getting or giving someone HIV (AIDS) or any other STD, such as chlamydia, gonorrhea, genital warts or herpes.
SIDE EFFECTS
Irregular Bleeding:
The most common side effect of POPs is a change in menstrual bleeding. Your periods may be either early or late, and you may have some spotting between periods. Taking pills late or missing pills can result in some spotting or bleeding.
Other Side Effects:
Less common side effects include headaches, tender breasts, nausea and dizziness. Weight gain, acne and extra hair on your face and body have been reported, but are rare.
If you are concerned about any of these side effects, check with your doctor or clinic.
USING POPs WITH OTHER MEDICINES
Before taking a POP, inform your health care provider of any other medication, including over-the-counter medicine, that you may be taking.
These medicines can make POPs less effective:
Medicines for seizures such as:
- Phenytoin (Dilantin)
- Carbamazepine (Tegretol)
- Phenobarbital
Medicine for TB:
- Rifampin (Rifampicin)
Before you begin taking any new medicines be sure your doctor or clinic knows you are taking a progestin-only birth control pill.
HOW TO TAKE POPs
IMPORTANT POINTS TO REMEMBER
- POPs must be taken at the same time every day, so choose a time and then take the pill at that same time every day. Every time you take a pill late, and especially if you miss a pill, you are more likely to get pregnant.
- Start the next pack the day after the last pack is finished. There is no break between packs. Always have your next pack of pills ready.
- You may have some menstrual spotting between periods. Do not stop taking your pills if this happens.
- If you vomit soon after taking a pill, use a backup method (such as a condom and/or a spermicide) for 48 hours.
- If you want to stop taking POPs, you can do so at any time, but, if you remain sexually active and don't wish to become pregnant, be certain to use another birth control method.
- If you are not sure about how to take POPs, ask your doctor or clinic.
STARTING POPs
- It's best to take your first POP on the first day of your menstrual period.
- If you decide to take your first POP on another day, use a backup method (such as a condom and/or a spermicide) every time you have sex during the next 48 hours.
- If you have had a miscarriage or an abortion, you can start POPs the next day.
IF YOU ARE LATE OR MISS TAKING YOUR POPs
-
If you are more than 3 hours late or you miss one or more POPs:
- TAKE a missed pill as soon as you remember that you missed it,
- THEN go back to taking POPs at your regular time,
- BUT be sure to use a backup method (such as a condom and/or a spermcide) every time you have sex for the next 48 hours.
- If you are not sure what to do about the pills you have missed, keep taking POPs and use a backup method until you can talk to your doctor or clinic.
IF YOU ARE BREASTFEEDING
- If you are fully breastfeeding (not giving your baby any food or formula), you may start your pills 6 weeks after delivery.
- If you are partially breastfeeding (giving your baby some food or formula), you should start taking pills by 3 weeks after delivery.
IF YOU ARE SWITCHING PILLS
- If you are switching from the combined pills to POPs, take the first POP the day after you finish the last active combined pill. Do not take any of the 7 inactive pills from the combined pill pack. You should know that many women have irregular periods after switching to POPs, but this is normal and to be expected.
- If you are switching from POPs to the combined pills, take the first active combined pill on the first day of your period, even if your POPs pack is not finished.
- If you switch to another brand of POPs, start the new brand anytime.
- If you are breastfeeding, you can switch to another method of birth control at any time, except do not switch to the combined pills until you stop breastfeeding or at least until 6 months after delivery.
PREGNANCY WHILE ON THE PILL
If you think you are pregnant, contact your physician. Even though research has shown that POPs do not cause harm to the unborn baby, it is always best not to take any drugs or medicines that you don't need when you are pregnant.
You should get a pregnancy test:
- If your period is late and you took one or more pills late or missed taking them and had sex without a backup method.
- Anytime it has been more than 45 days since the beginning of your last period.
WILL POPs AFFECT YOUR ABILITY TO GET PREGNANT LATER?
If you want to become pregnant, simply stop taking POPs. POPs will not delay your ability to get pregnant.
BREASTFEEDING
If you are breastfeeding, POPs will not affect the quality or amount of your breastmilk or the health of your nursing baby.
OVERDOSE
No serious problems have been reported when many pills were taken by accident, even by a small child, so there is usually no reason to treat an overdose.
OTHER QUESTIONS OR CONCERNS
If you have any questions or concerns, check with your doctor or clinic. You can also ask for the more detailed "Professional Labeling" written for doctors and other health care providers.
HOW TO STORE YOUR POPs
Store at 25°C (77°F); excursions permitted to 15°-30°C (59°-86°F).
PHARMACEUTICAL, INC.
Raritan, New Jersey 08869
©OMP 1998 REVISED JANUARY 2002 635-50-894-2
-
MODE OF ACTION
Subscribe to the "News" RSS Feed 
TOP ۞
